Snakebites in the Field
In Europe and North America more people die from bee and wasp stings than snake bites. Yet a snake bite in a survival situation is a nasty thing to contemplate. A bite can be life threatening; and unfortunately, only hospital care can improve the chances for survival of the person and to reduce the aftereffects of a bite. However failure to take preventive measures or failure to treat snakebite properly in a survival situation can result in needless illness.
Care of Snakebites in the Field
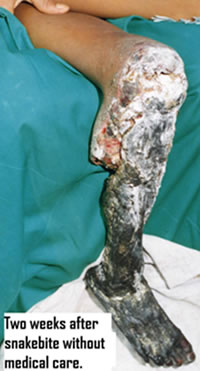 Deaths from snakebites are rare. Although all bites by poisonous snakes must be considered medical emergencies until it is proven that envenomation has not occurred, many such bites will prove not to be life threatening because the snake did not inject venom. No envenomation occurs in approximately 20% of documented bites by New-World pit vipers - rattlesnake, copperhead, water moccasin, and fer-de-lance. An even higher percentage of bites inflicted by other snake families (e.g., up to 50% for cobras and 75% for sea snakes) are "dry."
Deaths from snakebites are rare. Although all bites by poisonous snakes must be considered medical emergencies until it is proven that envenomation has not occurred, many such bites will prove not to be life threatening because the snake did not inject venom. No envenomation occurs in approximately 20% of documented bites by New-World pit vipers - rattlesnake, copperhead, water moccasin, and fer-de-lance. An even higher percentage of bites inflicted by other snake families (e.g., up to 50% for cobras and 75% for sea snakes) are "dry."
The most common complication of pit viper snakebites is called Compartment Syndrome (in which increased pressure caused by inflammation and tissue swelling within a confined space in the body impairs blood supply, leading to nerve damage and muscle death). This can be a direct result of the snakebite or also from misapplication of a constriction band. Snakebite can also lead to:
- Local wound complications that may include infection and skin loss.
- Cardiovascular complications, blood disorders, and pulmonary collapse may occur.
- Prolonged neuromuscular blockade may occur from coral snake envenomations.
Most viper bites contain hemotoxic elements which damage tissue and affect the circulatory system by destroying skin tissues and causing internal hemorrhaging. Viper venom also contains neurotoxic components which immobilize the nervous system, affecting the victim's breathing, sometimes stopping it. Most vipers have venom composed primarily of hemotoxic properties. Baby rattlesnakes and the Mojave Rattler are an exception; they have venom which contains more neurotoxic properties than hemotoxic -- which makes them very dangerous. The Sea Snake, Coral Snake, and Cobra family of snakes also have venom with dominant neurotoxic characteristics but they too have hemorrhagic toxins. The venoms also contain digestive enzymes (cytotoxins) to aid in digesting their prey. When you have been bitten, the venom also begins to digest you from within (Happy thought). These venoms can cause a very large area of tissue death, leaving a large open wound. This condition could lead to the need for eventual amputation if not treated.
Signs & Symptoms
A snakebite, whether from a venomous or non-venomous snake, usually causes terror, with nausea, vomiting, rapid heartbeat, diarrhea, profuse sweating, which may be difficult to distinguish from signs of true envenomation.
Shock and panic in a person bitten by a snake can also affect the person's recovery. Excitement, hysteria, and panic can speed up the circulation, causing the body to absorb the toxin quickly. Signs of shock may occur within the first 30 minutes after the bite.
Pit vipers, such as rattlesnakes, cotton mouth (water moccasins), copperheads, Fer-de-lance and bushmasters are the most common venomous snakebites in the Americas. Many pit viper bites are dry (venom is not deposited), and no systemic symptoms or signs develop.
Some of the signs of envenomation may include:
- Bleeding from the site.
- Fang mark(s) and scratch(es).
- If envenomation has occurred, swelling and redness of skin or bruising at the bite site and adjacent tissues will occur, usually within 30 to 60 min.
- Pain, tingling or burning at the area of the bite.
- Some rattlesnake bite victims develop a rubbery, minty, or metallic taste in their mouth.
- The venom of most North American pit vipers produces minor neuromuscular conduction changes, including generalized weakness and a sensation of tingling, pricking, or numbness of the person's skin.
- Blurred vision, weakness, dizziness and fainting, nausea, difficulty breathing.
- Swelling progresses rapidly and may involve the entire extremity within hours.
- Enlarged, tender regional lymph nodes may develop.
- Temperature increases over the bite area.
- In moderate or severe envenomations, bruising & discoloration is common and may appear at and around the bite site within 3 to 6 hours.
- Bruising & discoloration is most severe after bites by Eastern and Western diamondbacks; cottonmouths; and prairie, Pacific, and timber rattlesnakes.
- Bruising& discoloration is less common after copperhead and Mojave rattlesnake bites.
- The skin around the bite may appear tense and discolored.
- Blisters, of watery liquid or blood or both, usually appear at the bite site within 8 hours.
- Necrosis around the bite site is common after rattlesnake envenomations.
- Most venom effects on soft tissues peak within 2 to 4 days.
NOTE: Neurotoxins such as the Mojave rattlesnake, coral snakes, etc are a particularly dangerous for its ability to inflict severe, even fatal, injury without any appreciable degrees of pain or swelling; patients bitten often do not exhibit these signs and symptoms because its venom is more neurotoxic than that of the average pit viper. The absence of local symptoms and signs may erroneously suggest a dry bite, producing a false sense of security for the victim. Weakness of the bitten extremity may not become evident for 12 hours or more. Systemic neuromuscular disorders may be delayed for 12 hours and include weakness and lethargy; altered mental state, including euphoria and drowsiness, blurred vision, slurred speech, and difficulty swallowing; increased salivation; and respiratory distress or failure. Once the neurotoxic venom effects manifest, they are difficult to reverse and may last 3 to 6 days. Untreated patients may die of respiratory failure.
Care
The only proven therapy for snakebites is antivenom! Antivenom neutralizes the venom and has to be started within hours of the bite. Unless you have a portable emergency room with lab support, and a doctor along, forget about carrying the IV solutions, 10-20 vials of antivenom for vipers or the 10 possibly needed neurotoxin snakes. The person needs critical care and promptly!
The phrase "first, do no harm" has significant meaning here because many poor attempts at first-aid may do more harm than good; including things like making an incision over the bite, mouth suctioning, tourniquets, ice packs, or electric shock. A primary concern in the treatment of snakebite is to limit the amount of eventual tissue destruction around the bite area.
If you determine that a poisonous snake did bite an individual, take the following steps:
- "In the field, the victim should move or be moved beyond the snake's striking distance. Many snakes will not travel more than 20 feet after biting a person.
- The victim should avoid exertion and be reassured, kept warm and rapidly transported to the nearest medical facility.
- A bitten extremity should be loosely immobilized in a functional position just below heart level.
- All rings, watches, and constrictive clothing should be removed.
- Some providers strongly advocate the use of pressure-immobilization techniques only for snakebites caused by neurotoxic-predominant species. However, other providers advocate pressure-immobilization for all venomous snakebites; however, pressure immobilization may cause arterial insufficiency and necrosis if applied improperly.
- If it can be placed within 30 minutes, a pressure wrap (e.g. Ace Bandage) is placed above the bite about 2-4 inches. The wrap should be just tight enough to impede lymphatic flow, thereby delaying the systemic absorption and circulation of the venom but not so tight to restrict venous or arterial circulation; snug as if applying a bandage for a sprain, yet able to slide a finger under the bandage. As swelling progresses, the bandage may need to be reapplied to prevent compressing the tissues.
- Set up for shock and force fluids or give by intravenous (IV) means.
- Maintain an airway (especially if bitten near the face or neck) and be prepared to administer mouth-to-mouth resuscitation or CPR.
- Wash the bite with clean water and soap or antiseptic swabs. While washing look for embedded fangs or teeth in the wounds.
- Immobilize the bitten area and keep it lower than the heart.
- If hospitalization will be more than 30 minutes, a suction device (The Extractor from Sawyer Products) may be placed over the bite to help draw venom out of the wound without making cuts.
- In the USA, identifying the snake is not a concern as it once was, due to the new antivenom is now designed for all pit vipers in the country. Trying to kill a snake is dangerous. A rattlesnake can strike and bite for more than an hour after its death.
NOTE: Snake toxin is not inactivated by changes in temperature or pH. Application of ice, hot packs, or vinegar only wastes time. All other out-of-hospital interventions (e.g., tourniquets, topical preparations, suction by mouth or with a device with incision, cryotherapy, and electrical shock) are of no proven benefit, may be harmful, and may delay appropriate treatment.
DO NOT
- Do not cut the bite. Cutting opens capillaries that in turn open a direct route into the blood stream for venom and infection.
- Do not apply a tourniquet. Such action can result in the loss of the limb.
- Do not try to suck out the venom by mouth. You can try the suction cup in a snakebite kit if it doesn't delay other needed treatment. Suctioning seldom provides any measurable advantages, however.
- Do not apply cold and/or ice packs. Recent studies indicate that application of cold or ice makes the injury much worse.
- Do not give the victim stimulants, alcoholic beverages or tobacco products.
- Do not give blood thinners such as aspirin or acetaminophen.
- Do not put your hands on your face or rub your eyes, as venom may be on your hands. Venom may cause blindness.
- Do not break open the large blisters that form around the bite site.
Follow-up Care
A snakebite wound can become infected from bacteria in its mouth. With nonpoisonous as well as poisonous snakebites, this local infection is responsible for a much of the damage that can result later.
- If infection appears, keep the wound open and clean.
- Use heat after 24 to 48 hours to help prevent the spread of local infection. Heat also helps to draw out an infection.
- Keep the wound covered with a dry, sterile dressing.
- Have the victim drink large amounts of fluids until the infection is gone.
-Jerry B Blaine
Comments
Customer reviews
No posts found
